Updated 8 November 2023 | Approved By Dr. Umberto Russo
What is Lymphoedema?
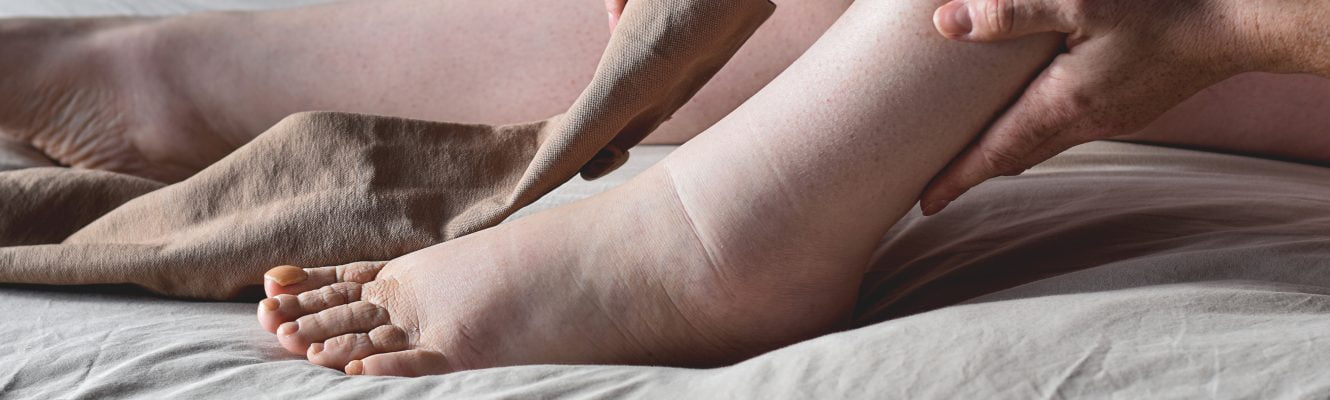
Lymphoedema is a condition where your body has difficulty getting rid of a fluid called lymph. This fluid helps clean your body and keep it healthy. However, problems can arise after certain events or conditions, such as surgery or injury. As a result, fluid starts to build up, usually in your arms or legs. Swelling around these areas can occur and progressively worsen over time. People with lymphoedema often need special therapy or massages to help reduce the swelling and make life more comfortable.Lymphoedema Symptoms and Signs
Lymphoedema is a condition characterised by the buildup of lymphatic fluid in body tissues, leading to swelling. The symptoms of lymphoedema can include [2]:- Persistent swelling that usually occurs in the arm or leg. Swelling may vary in severity and can range from mild to quite pronounced.
- Heaviness or fullness in the affected limb.
- Tightness or discomfort.
- Decreased flexibility and mobility.
- The skin over the swollen area may become thicker and harder.
- Increased risk of infections due to poor lymphatic drainage.
Lymphoedema Causes
Lymphoedema happens when your body's lymphatic system isn’t working effectively. This system is responsible for clearing out extra fluid and waste from your body. There are a few common reasons why lymphoedema can occur [3]:- Surgery: Sometimes, surgery to remove lymph nodes or treat cancer can affect the flow of lymph fluid, leading to lymphoedema.
- Radiation Therapy: If you've had radiation therapy as part of cancer treatment, it can harm the lymphatic system and cause swelling.
- Infection: Infections can mess up your lymphatic system, and if they happen near your lymph nodes, it might trigger lymphoedema.
- Inherited: In some cases, lymphoedema can be passed down through families, which means you're born with it.
- Obesity or Inactivity: Being overweight or not moving around much can strain your lymphatic system and potentially lead to lymphoedema.
- Injury: Sometimes, an injury, like a bad cut or a burn, can damage your lymphatic vessels, causing swelling.
Lymphoedema Diagnosis and Testing
GPs will often conduct thorough testing to determine a lymphoedema diagnosis. If your doctor confirms that you have lymphoedema, they'll work with you to develop a management plan. It's important to get an early diagnosis and start managing it to help prevent complications. Also, if you suspect you might have lymphoedema or are at risk, don't hesitate to reach out to a healthcare professional for evaluation and guidance. Common assessments include [2]:Physical Examination
Your GP will check your body for signs of swelling and its extent. Additionally, information about your medical history and any past surgeries or treatments can be important clues. They might also gently press on your skin to see if it leaves an indentation, which can be a sign of lymphoedema. Additionally, your GP will assess the size of both your affected and unaffected limbs to see the difference in size.Imaging Tests
In some cases, they might use imaging tests like ultrasound or lymphoscintigraphy. These tests help get a closer look at your lymphatic system and how it's working.Lymphatic Function Tests
Specialised tests may be done to check how well your lymphatic system is functioning. Examples of these tests include lymphoscintigraphy, lymphangiography, duplex ultrasonography, etc.Lymphoedema Treatment
GPs play an integral role in recommending treatment for lymphoedema. It is important that you are referred to other healthcare professionals, such as physiotherapists and occupational therapists, to develop a personalised treatment plan. Regular monitoring and proper self-care are key to managing lymphoedema effectively and improving your quality of life. Treatments include [4]:Compression Garments
Wearing specially designed compression garments, like sleeves or stockings, can help reduce swelling by applying gentle pressure on the affected limb. These garments are custom-fitted and can be an essential part of managing lymphoedema.Manual Lymphatic Drainage
This is a specialised massage technique performed by trained therapists. It helps stimulate lymph flow and reduce swelling.Exercise
Gentle, targeted exercises can assist in moving lymph fluid and improving the flexibility and strength of the affected limb. A physiotherapist can provide guidance on suitable exercises. Maintaining a healthy weight and avoiding prolonged sitting or standing can help manage lymphoedema.Skin Care
Keeping the skin clean and well-moisturised is crucial to prevent infections. Avoiding cuts, burns, and insect bites is also important.Psychological Support
Living with a chronic condition can be emotionally challenging, so seeking psychological support and connecting with support groups can be beneficial.Surgery
In some cases, when conservative treatments aren't effective, surgical options may be considered. There are different surgical procedures, such as lymphatic vessel transplantation or liposuction, aimed at improving lymphatic flow or reducing excess tissue. Surgery is typically reserved for severe cases and should be discussed with a healthcare specialist to determine the most suitable approach.Lymphoedema Complications
Lymphoedema is a condition where excess fluid accumulates in your tissues, causing swelling, usually in an arm or leg. If not properly managed, it can lead to various complications [5]. To avoid these complications, it's crucial to work closely with healthcare professionals, such as physiotherapists, occupational therapists, and lymphoedema specialists. They can help you develop a tailored management plan that may include exercises, compression garments, skin care, and other strategies to minimise the risk of complications and improve your overall health and comfort.Infection
Lymphoedema can make your skin more vulnerable to infections, like cellulitis. It's important to keep the skin clean and take precautions to prevent these infections.Skin Changes
Over time, the skin in the affected area can become thicker, hard, and prone to developing warts or other skin problems.Reduced Mobility
Severe swelling can limit your ability to move the affected limb, affecting your daily activities and quality of life.Psychological Impact
Dealing with a chronic condition like lymphoedema can be emotionally challenging. It's essential to seek support and guidance for managing the condition and its impact on your well-being.Receiving quality care from highly experienced doctors is essential for a prompt diagnosis and receiving the correct medical treatment. With 24-7 MedCare, you can experience telemedicine from the convenience of your own home. Our friendly online doctors will be available 24/7 for a consultation, anytime and anywhere in Australia.
To make a telehealth appointment booking, simply click on the button below.
References
- AIHW (Australian Institute of Health and Welfare). (2023). Prevalence of Lymphoedema in Australia. Retrieved from https://www.aihw.gov.au/reports/chronic-disease/prevalence-of-lymphoedema-in-australia/summary
- Lymphoedema Support Network (LSN). (n.d.). What Is Lymphoedema? Retrieved from https://www.lymphoedema.org.au/about-lymphoedema/what-is-lymphoedema/#Early%20warning%20signs
- Grada, A. A., & Phillips, T. J. (2017). Lymphedema: Pathophysiology and clinical manifestations. Journal of the American Academy of Dermatology, 77(6), 1009-1020.
- Cancer Council. (n.d.). Lymphoedema: Treatment and Management. Retrieved from https://www.cancercouncil.com.au/cancer-information/managing-cancer-side-effects/lymphoedema/treatment-and-management/
- National Center for Biotechnology Information. (2019). Lymphedema. Retrieved from https://europepmc.org/article/nbk/nbk537239/